Master the T/C ratio method, learn when to start testing, and time intercourse perfectly for conception.
Key takeaways
- Your fertile window is only 6 days - 5 days before ovulation plus ovulation day (12-24 hour egg lifespan).
- Start testing on cycle day (length - 17) - this formula prevents wasting tests or missing your surge.
- Positive = T/C ratio >= 1:1 - test line as dark as control line means LH surge detected (ovulation in 24-36 hours).
- Test between 10 AM - 8 PM, not first morning urine - LH surges begin in early morning, afternoon urine catches it.
- Have intercourse every other day after positive - covers fertile window while maintaining sperm quality.
- 97-99% accurate when used correctly - but 7-10% of LH surges do not result in actual ovulation.
- Combine with BBT and cervical mucus for confirmation - the triple-check method validates your fertile window.
Ovulation tests detect the luteinizing hormone (LH) surge that occurs 24-36 hours before your egg is released, giving you a precise window to time intercourse for conception. Unlike guessing based on calendar apps alone, these at-home tests measure the actual hormonal shift that triggers ovulation. This guide teaches you the medical-standard T/C ratio method used by fertility clinics, so you can stop second-guessing faint lines.
In this guide
Understanding your fertile window: the 6-day rule
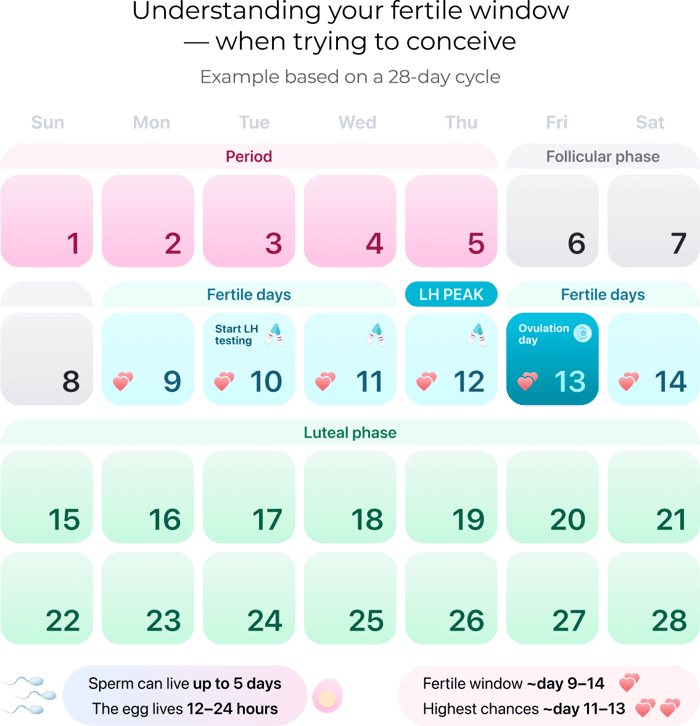
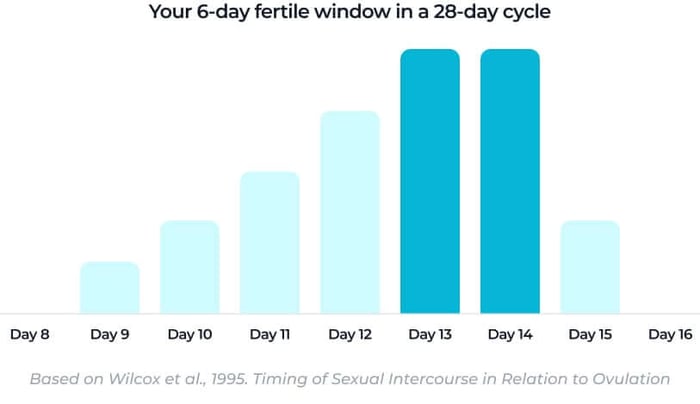
Your fertile window is the only time each cycle when pregnancy can occur, and it is shorter than most people think. This window includes:
- 5 days before ovulation - sperm can survive up to 5 days in fertile cervical mucus.
- The day of ovulation itself - the egg lives for only 12-24 hours after release.
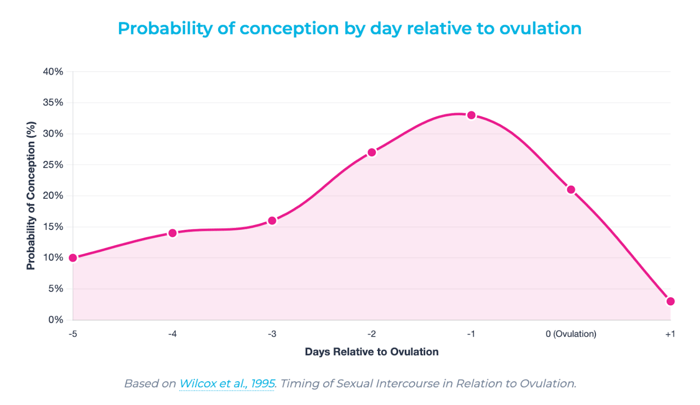
Why timing matters: Missing this window means waiting another full cycle. Since sperm need time to travel and capacitate, having intercourse before the egg is released is actually more effective than waiting until ovulation day. Research shows the highest pregnancy rates occur with intercourse 1-2 days before ovulation.

What ovulation tests actually measure (and why it works)
Ovulation predictor kits (OPKs) work by detecting luteinizing hormone (LH) in your urine. Here is the science:
- LH triggers ovulation: 24-36 hours before your ovary releases an egg, your pituitary gland releases a surge of LH.
- The surge is detectable: LH levels spike from baseline (5-20 mIU/mL) to peak (25-100+ mIU/mL).
- Urine concentration reflects blood levels: what is in your bloodstream shows up in your urine within hours.
The T/C ratio explained
Professional fertility clinics use the test-to-control line ratio (T/C ratio) as the gold standard. A positive result means T/C >= 1:1, meaning the test line is as dark as or darker than the control line. This indicates LH levels have crossed the threshold for ovulation.
Why T/C ratio matters
Many women waste time waiting for a "super dark" line. The truth: as soon as the test line matches the control line in intensity, your LH has surged. This is your signal to time intercourse. Do not wait for it to get darker, or you might ovulate before you act.
Quick takeaway
Ovulation tests catch the hormone spike (LH) that happens 24-36 hours before your egg drops. When the two lines match in darkness, that is your green light - time to have sex today, tomorrow, and the day after.
Types of ovulation tests
| Test Type | How It Works | Pros | Cons |
|---|---|---|---|
| Strip Tests | Dip in urine cup; compare lines by eye | Affordable ($0.30-0.50/test), test 2x/day, track T/C progression | Requires line interpretation |
| Digital Tests | Insert in urine stream; displays symbol | Easy to read (smiley face = positive) | Expensive ($3-5/test), no gradual tracking |
| Advanced Digital | Measures estrogen + LH | Identifies up to 6 fertile days | Most expensive, more complex |
Best for most women: Strip tests offer the best value for frequent testing and allow you to track LH progression visually, which is helpful for learning your unique pattern.
Get accurate results without breaking the bank
Pregmate 50-count and 100-count ovulation test strips offer clinical-grade accuracy at $0.30-0.50 per test, perfect for daily or twice-daily testing. All tests use the medical-standard T/C ratio method trusted by fertility clinics.
When to start testing (the "minus 17" rule)
Generic advice usually says "start on Day 10," but this often leads to wasted tests or missed surges.
Because ovulation typically happens 14 days before your next period, the best time to start testing is 17 days before your next expected period. This gives you a 3-day buffer to catch the LH rise before it peaks.
Calculate your start day
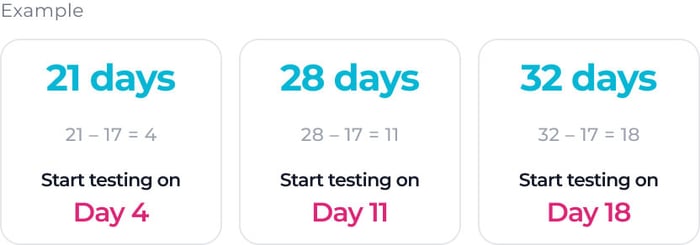
Formula: Cycle Length - 17 = Start Day
- Count the days from the first day of your last period to the first day of your next period (this is your cycle length).
- Subtract 17 from that number.
- Start testing on that cycle day.
Example: 32-day cycle -> 32 - 17 = Day 15 (start testing on Day 15).
What if your cycle is irregular?
Start testing on Day 6 and continue daily until you get a positive or your period starts. Yes, you will use more tests, but missing ovulation costs you a whole month.
When cycles vary by 7+ days: consider testing twice daily (morning and evening) during your estimated fertile window to catch short LH surges that last less than 24 hours.
Quick takeaway
Do not start testing on Day 10 like everyone says. Take your cycle length, subtract 17, and that is your start day. Example: 30-day cycle? Start on Day 13. Irregular? Start on Day 6 and keep going until you get a positive or your period arrives.
How to read ovulation tests: the T/C ratio method
Stop second-guessing faint lines. Here is the objective standard:

- Negative (not yet fertile): Test line lighter than control line (T/C ratio < 1:1). LH is present but has not surged yet. Action: Keep testing daily.
- Positive (peak fertility): Test line as dark as or darker than control line (T/C ratio >= 1:1). LH surge detected. Action: Have intercourse today, tomorrow, and the day after.
Common mistake
Waiting for the test line to be "very dark." Even if the lines are equal in intensity, that is positive. Do not wait for a super-dark line, or you might ovulate and miss your window.
Quick takeaway
If the test line is lighter than the control line, keep testing. If they match or the test line is darker, you are likely ovulating in 24-36 hours. That is your go-time.
Digital test interpretation
- Empty circle or blank: Negative
- Smiley face or "Yes": Positive (LH surge detected)
- Flashing smiley (advanced tests): High estrogen detected - fertility rising but not yet peak
Testing protocol: maximize accuracy
Best time of day to test
10 AM - 8 PM is ideal. Here is why:
- LH surges often begin in the early morning.
- First morning urine (FMU) may miss the surge because it is concentrated overnight before the surge started.
- Mid-morning to evening urine reflects real-time LH levels.
Testing twice daily strategy: If you have short cycles or unpredictable ovulation, test at 10 AM and 6 PM. The surge can be as brief as 12-14 hours, so twice-daily testing helps you catch it.
Fluid intake matters
- Do not chug water 2 hours before testing - diluted urine can cause false negatives.
- Normal hydration is fine.
- If your urine is very pale or clear, wait an hour and test again.
Hold time
2-hour urine hold is recommended (do not pee for 2 hours before testing). This concentrates LH for accurate detection.
Your daily testing checklist
- Test between 10 AM - 8 PM (not first morning urine).
- Hold urine for 2 hours before testing.
- Avoid drinking excessive water 2 hours before.
- Dip strip for 3-5 seconds (follow package instructions).
- Read results within 5-10 minutes.
- Log result in an app or paper calendar.
- If positive: have intercourse today and every other day for the next 4-6 days.
Quick takeaway
Test in the afternoon, do not chug water beforehand, and hold your pee for 2 hours. If you test at the same time each day after lunch, you are much more likely to catch your surge.
Combining methods: the triple-check approach
Ovulation tests are powerful, but combining them with other methods gives you confirmation and deeper insight:
1. Basal body temperature (BBT)
What it measures: Your resting body temperature rises 0.5-1°F after ovulation due to progesterone
How to use it: Take your temp first thing every morning before getting out of bed
Why combine: BBT confirms ovulation happened, while OPKs predict it will happen—together, they validate your fertile window
2. Cervical mucus observation
Fertile mucus looks like: Clear, stretchy, slippery (like raw egg whites)
Timing: Appears 1-2 days before LH surge and peaks at ovulation
Why combine: Gives you an early warning system—start testing more frequently when you see fertile mucus
3. Ovulation pain (mittelschmerz)
What it feels like: One-sided lower abdominal twinge or ache lasting hours to a day
When it occurs: At or just before ovulation
Why combine: Physical confirmation that ovulation is happening right now
Track all your fertility signs in one place
The free Pregmate app lets you log ovulation tests, BBT, cervical mucus, and symptoms, then shows you personalized insights about your fertile window. Get testing reminders based on your unique cycle length.
Timing intercourse: the every-other-day rule
Once you get a positive ovulation test:
🎯 Intercourse timing strategy
✅ Have intercourse the day of the positive test
✅ Continue every other day for the next 4-6 days
✅ This covers the entire fertile window while maintaining sperm quality
Why not every day? Sperm count and quality can drop with daily ejaculation. Every-other-day timing maintains high sperm count while still covering the fertile window.
Alternate approach (if you have specific timing needs): Have intercourse the day before ovulation, the day of ovulation, and the day after. This covers the 3 most fertile days but requires precise test reading.
Quick takeaway
Get a positive test? Have sex that day, skip tomorrow, have sex the next day, skip, and repeat for about a week. Every other day keeps sperm fresh and still covers your whole fertile window.
Troubleshooting: what if you never get a positive?
5 common reasons for persistent negative results
1. Testing too late in your cycle
The problem: You start testing on Day 14, but you actually ovulate on Day 11
The fix: Calculate start day using the formula above; err on the side of starting early
2. Short LH surge
The problem: Your LH surge lasts only 10-12 hours, and you're testing once daily
The fix: Test twice daily (12 hours apart) during your expected fertile window
3. Anovulatory cycles
The problem: Some cycles, you don't ovulate at all—especially common with PCOS, high stress, or perimenopause
The fix: Track for 3 months; if you never see a positive, consult a doctor for hormone testing
4. Low LH baseline
The problem: Your baseline LH is low, and your surge doesn't reach the test's detection threshold
The fix: Use ultra-sensitive tests (10-15 mIU/mL threshold) or fertility monitor with estrogen tracking
5. Testing window missed
The problem: Irregular cycles make it hard to predict when to test
The fix: Start testing earlier (Day 6) and continue for 14+ days if needed
When to see a doctor
If you've tracked for 3+ cycles with no positive test, or if you're over 35 and have been trying for 6+ months, get a fertility workup. Blood tests can measure LH, FSH, AMH (ovarian reserve), and progesterone levels to diagnose issues.
Quick takeaway
Never getting a positive test? You are usually either testing too late, your surge is too short, or you may not be ovulating every cycle. The most common fix is simply starting earlier.
Beyond testing: lifestyle factors that impact fertility
Even perfect ovulation timing can be undermined by lifestyle factors. Here is what actually matters based on research:
✓ Proven to help:
Maintain BMI 18.5-24.9: Both underweight and overweight status can disrupt ovulation
Limit alcohol to ≤3 drinks/week: Heavy drinking (7+ drinks/week) associated with reduced fertility
Prenatal vitamins with folate: Start 3 months before conception for neural tube defect prevention
Manage stress: Chronic high cortisol can delay or suppress ovulation
✗ Common myths to ignore:
Lying down after sex (sperm reach the cervix within seconds)
Specific sex positions (no evidence any position improves conception rates)
"Saving up" sperm by abstaining for weeks (sperm quality drops after 5-7 days)
Take control of your fertility journey
Whether you are just starting to try or you have been at it for months, consistent testing builds a clear picture of your unique fertility pattern.
Frequently asked questions
- Can I use ovulation tests as birth control?
- No. Ovulation tests detect the LH surge but do not tell you when your fertile window ends. Since sperm can survive 5 days, you could have intercourse before the LH surge and still conceive.
- How accurate are ovulation tests?
- When used correctly, ovulation tests are 97-99% accurate at detecting the LH surge. However, a positive test does not guarantee ovulation. About 7-10% of LH surges do not result in actual egg release.
- Can medications interfere with ovulation tests?
- Yes. Fertility medications containing hCG, such as Ovidrel or Pregnyl, can cause false positives because hCG is chemically similar to LH. Clomid and letrozole do not interfere.
- What does a faint line mean?
- A faint test line means LH is present but has not surged yet. Keep testing. Only when the test line matches or exceeds the control line (T/C >= 1:1) is it truly positive.
- Can I ovulate without an LH surge?
- It is rare but possible. Some women with very short surges may ovulate before the surge is detectable in urine. If you suspect this, test twice daily or use a fertility monitor.
- How long after a positive test are you actually fertile?
- You are fertile as soon as you get a positive test through roughly 24-48 hours after. Ovulation typically occurs 24-36 hours after the LH surge begins, and the egg lives for 12-24 hours.
Sources and references
- Mayo Clinic Press - Finding your fertility window
- Cleveland Clinic - Ovulation: Calculating, Timeline, Pain and Other Symptoms
- American Society for Reproductive Medicine - Optimizing natural fertility
- Ecochard, R., Duterque, O., Leiva, R., Bouchard, T., and Vigil, P. (2015). Self-identification of the clinical fertile window and the ovulation period.https://doi.org/10.1016/j.fertnstert.2015.01.031
- McGovern, P.G., Myers, E.R., Silva, S., et al. (2004). Absence of secretory endometrium after false-positive home urine luteinizing hormone testing.https://doi.org/10.1016/j.fertnstert.2004.04.070
- Wilcox, A.J., Weinberg, C.R., and Baird, D.D. (1995). Timing of Sexual Intercourse in Relation to Ovulation.https://doi.org/10.1056/NEJM199512073332301
- Johnson, S., Weddell, S., Godbert, S., Freundl, G., Roos, J., and Gnoth, C. (2015). Development of the first urinary reproductive hormone ranges referenced to independently determined ovulation day.https://doi.org/10.1515/cclm-2014-1087
Medical disclaimer: Ovulation tests are tools to assist with conception timing but should not replace consultation with a healthcare provider.
If you have been trying to conceive for 12 months (or 6 months if over age 35) without success, or if you have concerns about your menstrual cycle or fertility, please consult a reproductive endocrinologist or OB-GYN. Individual results may vary.